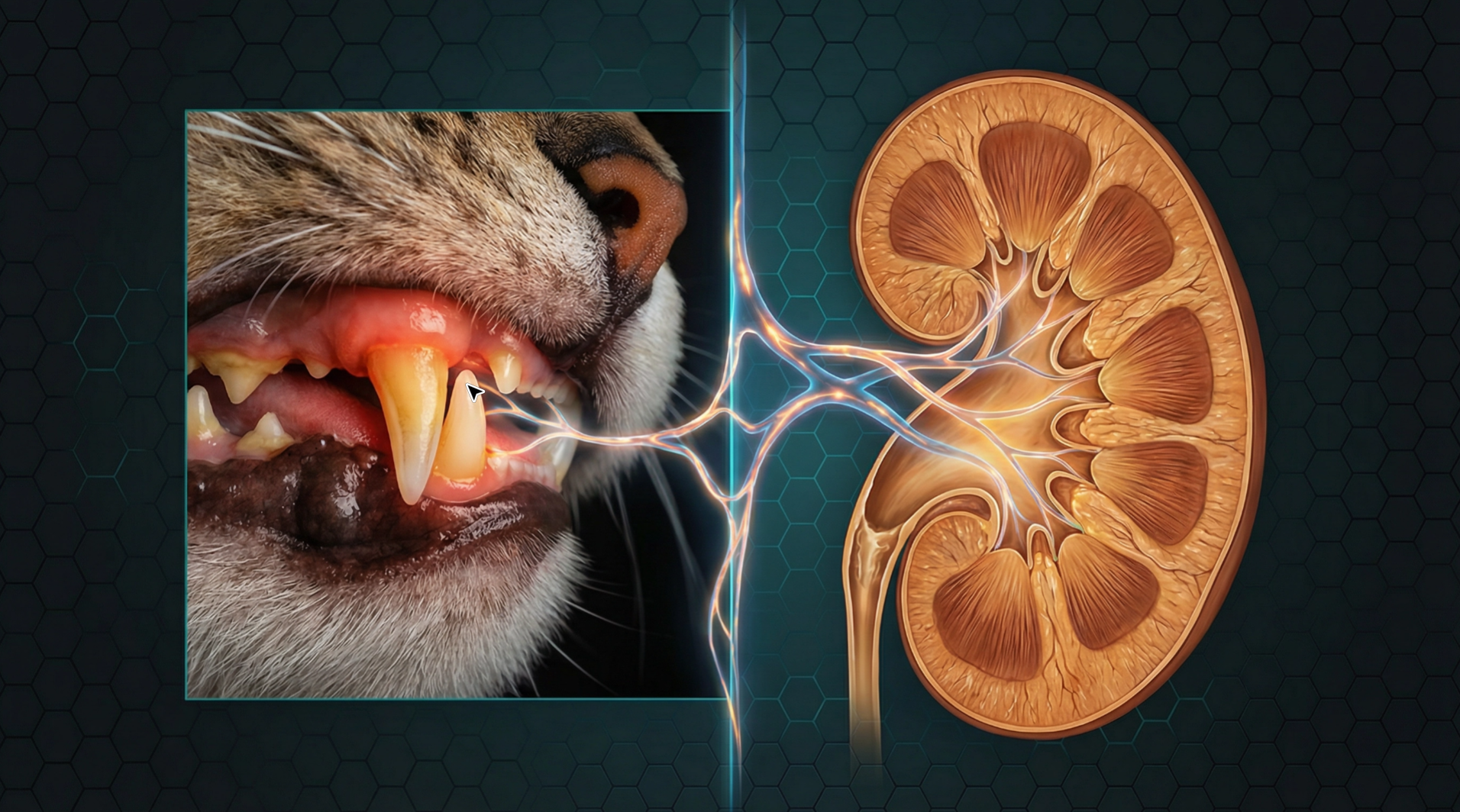
The Oral-Renal Axis and Chronic Kidney Disease in Companion Animals
Chronic kidney disease is a silent killer of aging cats and dogs, but its progression is closely linked to a surprising factor: oral health.
Jake Kelly
Pet Longevity Researcher
Objective: To provide a comprehensive review of the bidirectional relationship between oral health and chronic kidney disease (CKD) in canines and felines, and to outline current best practices for diagnosis, management, and emerging therapies.
Background: CKD is a leading cause of mortality in aging pets. The oral-renal axis — where periodontal inflammation accelerates CKD progression and uremia worsens oral health — is a critical concept for effective management. This brief synthesizes the pathophysiology of this axis and reviews the latest clinical guidelines.
Methods: This review consolidates information from peer-reviewed veterinary literature, consensus statements from the International Renal Interest Society (IRIS), and recent research on novel diagnostics and therapeutics. Topics covered include IRIS staging with creatinine and Symmetric Dimethylarginine (SDMA), dietary management (phosphorus restriction, omega-3s), hydration strategies, and the role of oral hygiene. The potential of emerging therapies, including AIM protein and stem cells, is also examined.
Results: The evidence strongly supports a multimodal management strategy for CKD. Early detection using SDMA allows for timely intervention. Dietary modification, particularly phosphorus restriction, remains the cornerstone of therapy, proven to slow disease progression. The review highlights the necessity of integrating professional and at-home dental care into CKD management protocols to mitigate the inflammatory burden of the oral-renal axis.
Conclusion: Acknowledging and addressing the oral-renal axis is fundamental to improving outcomes for pets with CKD. A proactive, integrated approach combining early diagnosis, nutritional science, diligent hydration, and comprehensive oral care can significantly extend both the quality of life and lifespan of animals affected by this common geriatric disease.
The Oral-Renal Axis and Chronic Kidney Disease in Companion Animals
Introduction
Chronic Kidney Disease (CKD) represents a final common pathway for numerous renal insults and is a major geriatric concern in veterinary medicine. It affects an estimated 30-40% of cats and 10% of dogs over the age of 10. The progression of CKD is often silent in its early stages, making early diagnosis and intervention critical for extending both lifespan and healthspan. Concurrently, periodontal disease is the most common infectious disease in companion animals, affecting over 80% of dogs and 70% of cats by age three. Historically viewed as separate conditions, recent research has illuminated a complex and clinically significant interplay between oral and renal health. This executive brief will explore the bidirectional nature of the oral-renal axis, detail best practices for CKD management, and provide a forward-looking perspective on novel therapies that promise to redefine outcomes for pets with kidney disease.
The Bidirectional Oral-Renal Axis
The oral-renal axis describes the bidirectional relationship where chronic oral inflammation, primarily from periodontal disease, contributes to the progression of CKD, and conversely, where CKD creates a uremic environment that exacerbates oral pathology. Periodontal disease, a state of chronic inflammation, allows bacteria and their endotoxins to enter the bloodstream, triggering a systemic inflammatory response. This chronic inflammation is a known risk factor for the progression of CKD in both humans and animals [3]. The kidneys, with their extensive vascular network, are particularly vulnerable to the effects of systemic inflammation and increased oxidative stress, which can lead to glomerulosclerosis and interstitial fibrosis, hallmarks of CKD [4].
Conversely, as CKD progresses, the accumulation of uremic toxins, such as urea and creatinine, in the bloodstream directly impacts oral health. The breakdown of urea in saliva to ammonia by urease-producing bacteria leads to a condition known as uremic stomatitis, characterized by painful oral ulcerations and a distinctive ammoniacal odor to the breath. Furthermore, the metabolic changes associated with CKD, including secondary renal hyperparathyroidism, can lead to demineralization of the jawbone (rubber jaw) and tooth mobility, further compromising oral health and function.
Diagnosing and Staging CKD: The IRIS System
Early and accurate diagnosis of CKD is foundational to effective management. The International Renal Interest Society (IRIS) has developed a globally recognized staging system based primarily on fasting blood creatinine concentrations, measured on at least two occasions in a stable, hydrated patient [7]. However, the integration of Symmetric Dimethylarginine (SDMA), a more sensitive biomarker for renal function, has revolutionized early detection. SDMA can detect as little as a 25% decrease in kidney function, often months or even years before creatinine levels rise above the normal range, which typically only occurs after a 75% loss of function [6]. The IDEXX SDMA test has become an invaluable tool, enabling veterinarians to identify pets in the earliest stages of kidney decline (IRIS Stage 1) and implement interventions sooner.
IRIS CKD Stage | Creatinine (mg/dL) - Dog | Creatinine (mg/dL) - Cat | SDMA (µg/dL) | Clinical Signs |
|---|---|---|---|---|
1 | < 1.4 | < 1.6 | > 14 | Usually none; diagnosis via persistent SDMA elevation or other renal abnormality. |
2 | 1.4 - 2.8 | 1.6 - 2.8 | 18 - 35 | Mild to moderate azotemia; clinical signs are often subtle or absent. |
3 | 2.9 - 5.0 | 2.9 - 5.0 | 36 - 54 | Moderate to severe azotemia; systemic clinical signs (e.g., anorexia, weight loss, vomiting) are common. |
4 | > 5.0 | > 5.0 | > 54 | Severe azotemia; high risk of systemic and life-threatening clinical signs. |
Sub-staging is also performed based on proteinuria (Urine Protein:Creatinine ratio) and blood pressure measurements, which further refines prognosis and treatment.
Management of CKD: A Multifaceted Approach
Beyond diet, the management of CKD involves a holistic strategy to maintain quality of life and slow disease progression. This includes ensuring adequate hydration, managing comorbidities, and addressing the oral health component of the oral-renal axis.
Dietary Intervention: The Cornerstone of CKD Management
Nutritional modification is the most critical intervention for slowing the progression of CKD. Therapeutic renal diets are designed to reduce the kidneys' workload and mitigate the metabolic consequences of renal failure. The primary goal is to control serum phosphorus levels, as hyperphosphatemia is a major driver of CKD progression and is associated with decreased survival times. Studies have repeatedly demonstrated that feeding a phosphorus-restricted diet can double the lifespan of cats and dogs with CKD [1].
Other key features of therapeutic renal diets include:
Modified Protein Levels: While historically focused on severe restriction, modern renal diets often employ moderate, high-quality protein to meet metabolic needs while reducing the production of nitrogenous waste products that contribute to uremia.
Omega-3 Fatty Acid Supplementation: Eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) from fish oil have been shown to reduce renal inflammation, lower glomerular pressure, and slow the decline in kidney function.
Increased Caloric Density: To combat the anorexia and muscle wasting common in later-stage CKD, these diets are often more calorically dense to ensure adequate energy intake.
Potassium and B-Vitamin Supplementation: To counteract increased urinary losses.
Buffering Agents: To help manage the metabolic acidosis that often develops in CKD patients.
Hydration: Maintaining Renal Perfusion
As kidney function declines, the ability to concentrate urine is lost, leading to polyuria (increased urination) and a compensatory polydipsia (increased thirst). Maintaining adequate hydration is crucial to prevent dehydration, which can cause a rapid decline in renal perfusion and precipitate an acute-on-chronic kidney crisis. Strategies to enhance water intake include:
Feeding wet food: Canned or fresh diets have a much higher moisture content than dry kibble.
Providing multiple water sources: Using different types of bowls and placing them in various locations can encourage drinking.
Water fountains: The movement and sound of a water fountain can be appealing to some pets, particularly cats.
Flavoring water: Adding a small amount of low-sodium chicken broth or tuna juice can make water more enticing.
In later stages of CKD (IRIS Stage 3 and 4), subcutaneous fluid therapy administered at home can be an effective way to maintain hydration and improve quality of life.
The Role of Oral Hygiene in CKD Management
Given the bidirectional nature of the oral-renal axis, a proactive approach to oral hygiene is a critical component of CKD management. For pets with existing CKD, a professional dental cleaning under anesthesia may be recommended to remove the source of chronic inflammation. While anesthesia in a patient with kidney disease requires careful management and monitoring, the benefits of removing a significant inflammatory load often outweigh the risks. Daily at-home dental care, including brushing with a pet-specific toothpaste, is the gold standard for preventing plaque and tartar accumulation. For pets unwilling to tolerate brushing, other options such as dental diets, water additives, and dental chews can be considered, although their efficacy is variable.
Emerging Therapies and Future Directions
The landscape of CKD treatment is on the verge of a significant transformation, with several novel therapies offering hope beyond traditional management. These cutting-edge approaches aim to not just slow the progression of the disease, but to potentially regenerate damaged kidney tissue and restore function.
AIM Protein Therapy: A Potential Cure for Feline CKD
A particularly exciting development for feline medicine is the work of Dr. Toru Miyazaki on the AIM (Apoptosis Inhibitor of Macrophage) protein. Dr. Miyazaki discovered that cats have a genetic anomaly that prevents their AIM protein from functioning correctly, leading to an inability to clear cellular debris from the kidney tubules. This accumulation of debris is a primary driver of CKD in cats. An injectable AIM therapy, designed to supplement this deficiency, is currently in development. Clinical trials are set to begin in 2025, with a potential market release as early as 2027 [5]. This therapy holds the promise of being a true disease-modifying treatment, and potentially a cure, for feline CKD, representing a paradigm shift in how we approach this devastating disease.
Stem Cell Therapy: Regenerative Potential
Regenerative medicine, particularly the use of mesenchymal stem cells (MSCs), is another promising frontier in CKD treatment. MSCs have potent anti-inflammatory and immunomodulatory properties and have been shown to home to sites of injury and promote tissue repair. In the context of CKD, MSC therapy aims to reduce renal inflammation and fibrosis, and to stimulate the regeneration of damaged kidney tissue. While still largely in the experimental stage, early studies in both dogs and cats have shown promising results, with improvements in kidney function and a reduction in clinical signs. Further research is needed to optimize protocols and determine long-term efficacy, but stem cell therapy represents a hopeful avenue for reversing, rather than simply managing, the damage caused by CKD.
Practical Guidance for Pet Owners
For the longevity-focused pet owner, a proactive and informed approach is key to managing CKD and leveraging the oral-renal connection for better health outcomes. Key action items include:
Prioritize Early and Regular Screening: Insist on annual or semi-annual wellness exams, especially for pets over seven years of age. Discuss SDMA testing with your veterinarian as a tool for early CKD detection, even in seemingly healthy animals.
Embrace a Dental Health Routine: The single most effective action you can take to protect both oral and renal health is to implement a daily dental care routine. Brushing your pet's teeth is the gold standard. If this is not feasible, discuss the most effective alternatives with your veterinarian.
Commit to Professional Dental Care: Schedule regular professional dental cleanings under anesthesia as recommended by your veterinarian. View this not as a cosmetic procedure, but as a critical medical intervention to remove a source of chronic, systemic inflammation.
Transition to a Renal Diet at the First Sign: If your pet is diagnosed with CKD, even in the earliest stages, work with your veterinarian to transition to a therapeutic renal diet. This is the most powerful tool for slowing disease progression.
Become a Hydration Expert: Actively monitor and encourage your pet's water intake. Utilize wet food, water fountains, and other strategies to ensure they stay well-hydrated.
Stay Informed on Emerging Therapies: Keep abreast of new developments in CKD research, such as AIM protein therapy for cats. Engage with your veterinarian about whether your pet might be a candidate for clinical trials or newly approved treatments as they become available.
Conclusion
The link between oral health and chronic kidney disease is no longer a topic of speculation but a clinically proven reality with profound implications for companion animal longevity. The oral-renal axis highlights the interconnectedness of systemic health and underscores the necessity of a holistic approach to veterinary care. By understanding this bidirectional relationship, pet owners and veterinarians can work together to implement strategies that not only manage existing kidney disease but also mitigate the risk of its development and progression. Through a combination of diligent oral hygiene, early and sensitive diagnostics like SDMA, evidence-based nutritional management, and a forward-looking perspective on emerging therapies, we can significantly improve the quality of life and extend the healthspan of our beloved canine and feline companions, turning the tide against one of the most common diseases of aging.
References
[1] Polzin, D. J. (2013). Evidence-based step-wise approach to managing chronic kidney disease in dogs and cats. Journal of veterinary emergency and critical care, 23(2), 205-215. https://onlinelibrary.wiley.com/doi/abs/10.1111/vec.12034
[2] Sparkes, A. H., Caney, S., Chalhoub, S., Elliott, J., Finch, N., Gajanayake, I., ... & Quimby, J. (2016). ISFM consensus guidelines on the diagnosis and management of feline chronic kidney disease. Journal of feline medicine and surgery, 18(3), 219-239. https://journals.sagepub.com/doi/abs/10.1177/1098612X16631234
[3] Glickman, L. T., Glickman, N. W., Moore, G. E., Lund, E. M., Lantz, G. C., & Pressler, B. M. (2011). Association between chronic azotemic kidney disease and the severity of periodontal disease in dogs. Preventive veterinary medicine, 99(2-4), 193-200. https://www.sciencedirect.com/science/article/abs/pii/S0167587711000298
[4] Hall, J. A., Yerramilli, M., Obare, E., Yerramilli, M., & Jewell, D. E. (2021). The impact of periodontal disease and dental cleaning procedures on renal and cardiac health in dogs. Plos one, 16(7), e0255310. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0255310
[5] Greycoat Research. (2025, March 27). Cat Kidney Disease Cure Nears Reality: Dr. Toru Miyazaki’s AIM Therapy Targets 2027. https://greycoatresearch.com/blogs/news/cat-kidney-disease-cure-nears-reality-dr-toru-miyazaki-s-aim-therapy-targets-2027
[6] IDEXX. (n.d.). Interpreting SDMA Test Results for Cats and Dogs. https://www.idexx.com/en/veterinary/reference-laboratories/sdma/interpreting-your-sdma-results/
[7] Brown, S., Elliott, J., Lefebvre, H., & Polzin, D. (2013). IRIS Staging of CKD. International Renal Interest Society. http://www.iris-kidney.com/guidelines/staging.html
Related Articles

The Ultimate Guide to Canine Longevity: Maximizing Healthspan in Senior Dogs
As our dogs age, the goal shifts from simply keeping them alive to maximizing their healthspan. This comprehensive guide breaks down the six science-backed pillars of canine longevity, from precision nutrition and hormone optimization to cognitive support and physical therapy. Discover actionable strategies and explore a real-world longevity supplement stack designed to target every major pathway of aging.

Ocular Degeneration & Hearing Loss in Aging Dogs
Comprehensive guide to age-related vision and hearing loss in dogs. Evidence-based prevention, supplements, and nutrition strategies to protect your senior dog's sensory health.

A Dog Owner's Guide to Chronic Kidney Disease: Diagnosis, Management, and Extending Life
Just received a kidney disease diagnosis for your dog? This guide breaks down everything a concerned owner needs to know about Chronic Kidney Disease (CKD), from understanding IRIS stages to the single most important action you can take: diet. Learn about the latest treatments that can extend your dog's life and how to partner with your vet to create the best care plan.